Today on the blog – in conjunction with Touro Infirmary – we are absolutely thrilled to be opening a dialog about sleep through our “Rest Assured: You Are Not Alone” series. As moms we are all often sleep deprived, and we struggle with making decisions around our children’s sleep habits as well. Should we use a crib or a bassinet? Is co-sleeping safe or not? Should we sleep train? And who IS the expert on sleep training anyway? Will the baby ever sleep more than 2 hours at a time? Why does my toddler have night terrors? When do I move the toddler to a “big kid” bed and oh my word why won’t they stay in the darn thing? Our goal through this series is to create a safe place for all of us to open up about the sleep issues that trouble us and to acknowledge that no matter our struggles or choices, we are never ever alone.
The challenges of sleep training a preemie
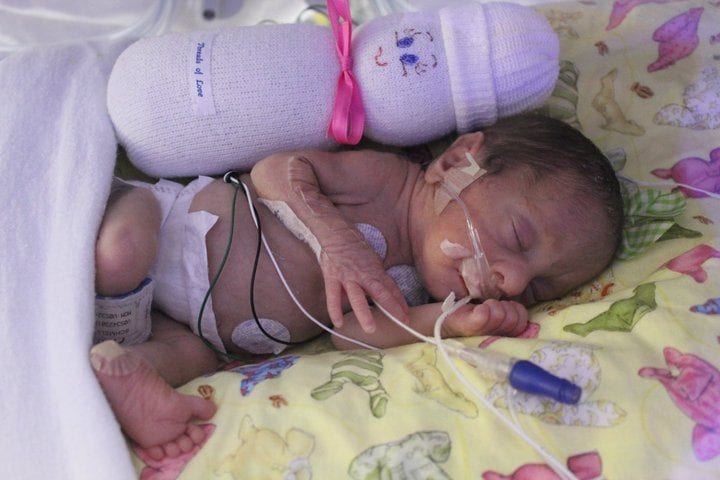 While Addison was in the hospital, the NICU nurses preached two main things to us: when she’s sleeping she’s growing and wake her every three hours to eat to ensure she’s getting all her calories.
While Addison was in the hospital, the NICU nurses preached two main things to us: when she’s sleeping she’s growing and wake her every three hours to eat to ensure she’s getting all her calories.
The night before Addison was discharged from the NICU, we had to “room in” at the hospital to make sure we knew how to use the oxygen concentrator and apnea monitor that would be coming home with us. The night went pretty smooth – none of the alarms were going off, and we followed the routine the wonderful nurses had already established, waking her every three hours to eat. We left the next morning with our itty bitty baby girl hooked up to an apnea monitor and travel oxygen tank. Forty minutes after we arrived home, a respiratory therapist showed up with the oxygen concentrator and more instructions. Talk about overwhelming! So many questions racing through our minds. We already had her feeding schedule worked out with enough formula to last the entire month, so the next thing to figure out was obviously sleep.
Where should she sleep?
We were hesitant to place Addison in her crib right away for a few different reasons:
- She didn’t even weigh five pounds when we were able to take her home.
- She had to sleep on an incline because of reflux issues.
- The tubing from the oxygen concentrator and wires from the apnea monitor made us a little nervous.
So we set up shop in the living room so to speak. One of us slept on the couch, while Addison slept in a Fisher Price bouncer on the floor. We would set our alarms to make sure she was being fed every three hours, and would take shifts so that one of us would get a good stretch of sleep in the bed.
 After a few weeks, we moved back into our bedroom, with the Rock N Play sleeper next to my side of the bed. I set up a small table with all of her feeding supplies, and we established a pretty good routine. After her 7pm feeding, she’d fall fast asleep until we had to wake her at 10pm to eat. We usually had to wake her again at 1am, but she almost always woke up at 4am by herself ready to eat. Most of the time, she’d go back down in the Rock N Play until 7am when we would try to keep her awake a little longer before she’d fall back asleep.
After a few weeks, we moved back into our bedroom, with the Rock N Play sleeper next to my side of the bed. I set up a small table with all of her feeding supplies, and we established a pretty good routine. After her 7pm feeding, she’d fall fast asleep until we had to wake her at 10pm to eat. We usually had to wake her again at 1am, but she almost always woke up at 4am by herself ready to eat. Most of the time, she’d go back down in the Rock N Play until 7am when we would try to keep her awake a little longer before she’d fall back asleep.
This worked well for a few months. Around four months old, our pediatrician told us we could let her eat on demand. We no longer had to wake her every three hours to eat. Praise the Lord! It was also around this time that our physical therapist said she should not be sleeping in the rock n play sleeper anymore because it would impede her head development, and we were already on watch for the right side of her head to round out a bit more. We were able to set up the pack n play in our room with a tucker sling so that she would be able to remain on an incline but on a firm surface.
Transitioning to the crib
Finally, one day when Addison was about six months old, while Michael was at work, I moved all of the equipment into her bedroom. She was still on the apnea monitor, but no longer on oxygen during the day. I set up the oxygen concentrator in the corner next to her crib so that the tubing would not get tangled with the apnea monitor at the foot of the crib. I figured what better time to move her to room while she had an apnea monitor attached, which would wake the neighbors if it went off in the middle of the night.
For the most part, Addison was a great sleeper and would wake up once during the night to eat. I wasn’t too worried about this since we still wanted to make sure she was getting enough calories. It wasn’t too long after, though, that she started sleeping through the night. She’d go down around 7:00pm and wake up around 6:00am.
The spica cast
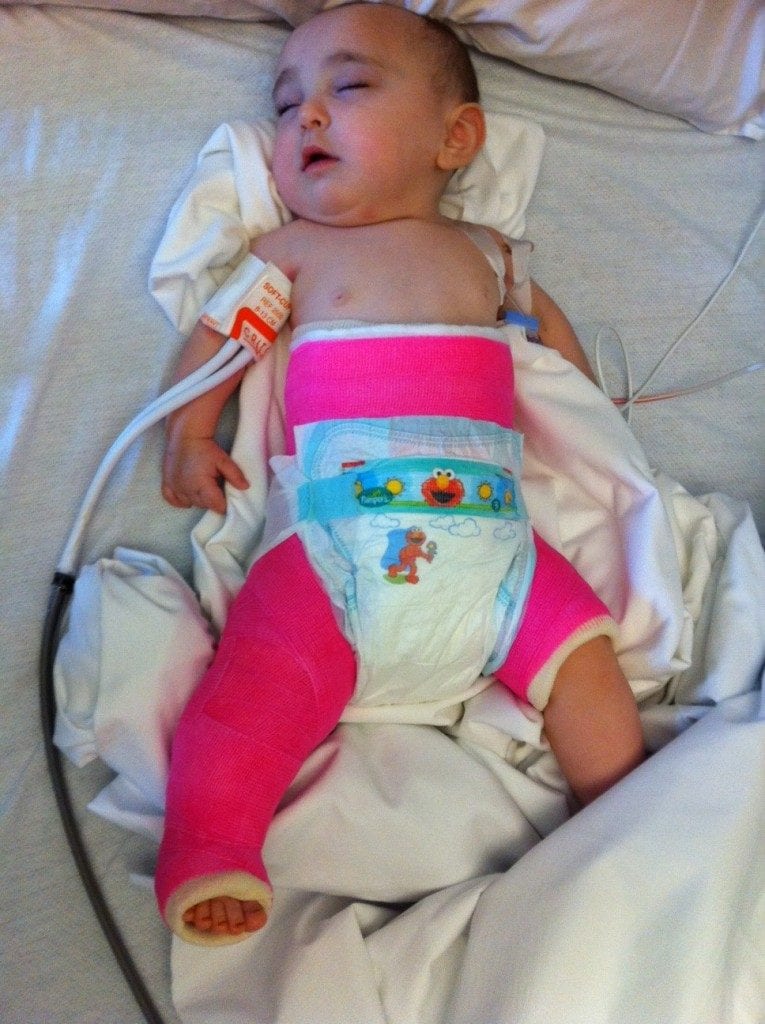 At eight months old, Addison had her 2nd hip surgery, an open reduction, which left her in a spica cast for seven weeks. Sleep was non-existent in our household. I felt terrible for our baby girl because I could only imagine how uncomfortable this cast was. We went into survival mode and did whatever we had to do to get sleep. Most of the time, this meant one of us slept on a recliner in the living room with Addison (and her 10 lb cast) sleeping on our chest. We prayed for the weeks to quickly pass. Unfortunately, she required another surgery and cast, which came off two weeks before her first birthday. She had been so used to sleeping with us, it had become a bad habit. At this point, I knew we had to do something. We all needed our sleep! Both Ashley & Andie recommended the Ferber method, so that very afternoon, I checked the book out of our local library. We waited until that weekend to put the sleep training into motion. The first night was rough. The second night was a tad bit better. The third night wasn’t bad at all. By the end of the next week, about eight days later, we were all sleeping through the night again!
At eight months old, Addison had her 2nd hip surgery, an open reduction, which left her in a spica cast for seven weeks. Sleep was non-existent in our household. I felt terrible for our baby girl because I could only imagine how uncomfortable this cast was. We went into survival mode and did whatever we had to do to get sleep. Most of the time, this meant one of us slept on a recliner in the living room with Addison (and her 10 lb cast) sleeping on our chest. We prayed for the weeks to quickly pass. Unfortunately, she required another surgery and cast, which came off two weeks before her first birthday. She had been so used to sleeping with us, it had become a bad habit. At this point, I knew we had to do something. We all needed our sleep! Both Ashley & Andie recommended the Ferber method, so that very afternoon, I checked the book out of our local library. We waited until that weekend to put the sleep training into motion. The first night was rough. The second night was a tad bit better. The third night wasn’t bad at all. By the end of the next week, about eight days later, we were all sleeping through the night again!
This past May, when she was 22 months old, she had her hopefully final hip surgery. This cast stayed on for twelve weeks, and during that time, there were no consistent sleep patterns in our house. We had transitioned to her toddler bed before her surgery since the weight and awkward position of the cast would cause difficulty lifting her over the front of the crib. Thankfully, that transition was pretty smooth. Toward the end of her time in the cast, we were all sleeping pretty well. We even had a few nights when she slept between ten and twelve hours! It was glorious!
These days
 These days, she is still in a toddler bed, sleeping pretty well for the most part. We have issues every now and then, especially if she isn’t feeling well or we’ve strayed from our bedtime routine. Our child is not one to sleep in if she goes to bed later than normal. What seems to happen, like on New Year’s Eve for instance, is she wakes up every couple of hours and is not in the best of moods the next day. Needless to say, because of that, we try to stay on schedule, with Addison going to bed between 7:30 and 8 each night.
These days, she is still in a toddler bed, sleeping pretty well for the most part. We have issues every now and then, especially if she isn’t feeling well or we’ve strayed from our bedtime routine. Our child is not one to sleep in if she goes to bed later than normal. What seems to happen, like on New Year’s Eve for instance, is she wakes up every couple of hours and is not in the best of moods the next day. Needless to say, because of that, we try to stay on schedule, with Addison going to bed between 7:30 and 8 each night.
We will be converting her bed to a full size bed really soon, and I’ve tried to involve her in all of her “big girl room” decorations to get her excited about the change. I think she’ll do fine with the transition. And since the mattress will be a tad bit bigger than the crib mattress she is currently sleeping on, if she does wake in the middle of the night, I’ll just climb right in the bed with her until she falls back asleep. Well, maybe…


















Great post. I slept on a cot in the nursery for 6 months after my micro preemie came home from the NICU because she had to be in her own room (away from her germ filled brothers) in a reclined chair. My daughter Joy was born at 23 weeks last year. Due to modern medicine and prayers she is doing great today. I hemorrhaged at 17 weeks for the first of 4 times because of 100% placenta previa, which turned into placenta accreta (which I believe was caused by 3 prior c-sections). After she came home from 121 days in the NICU, I wrote a memoir called “From Hope To Joy” about my life-threatening pregnancy and my daughter’s 4 months in the NICU (with my 3 young sons at home), which is now available on both the Amazon and Barnes&Noble websites. It was quite a roller coaster that I am certain some of you have been on or are currently riding on. My mission is to provide hope to women struggling with high-risk pregnancies, encourage expectant mothers to educate themselves before electing cesarean deliveries, provide families of premature babies a realistic look at what lies ahead in their NICU journey, and show that miracles can happen, and hope can turn into joy. Please see my website https://www.micropreemie.net and http://www.facebook.com/jenniferdegl and watch our amazing video of my daughter’s miracle birth and life at: https://www.youtube.com/watch?v=V_hleySg-iU
Thank you.