A Parents Guide to The NICU From a Neonatologist
Here at Touro we understand that the NICU may be a scary and confusing place for parents. As “the Place where Babies Come from” we know that having a baby in the NICU can be a stressful time and being in the middle of a global pandemic can only add to that. We are going to talk about what parents should expect while their baby is in the NICU, and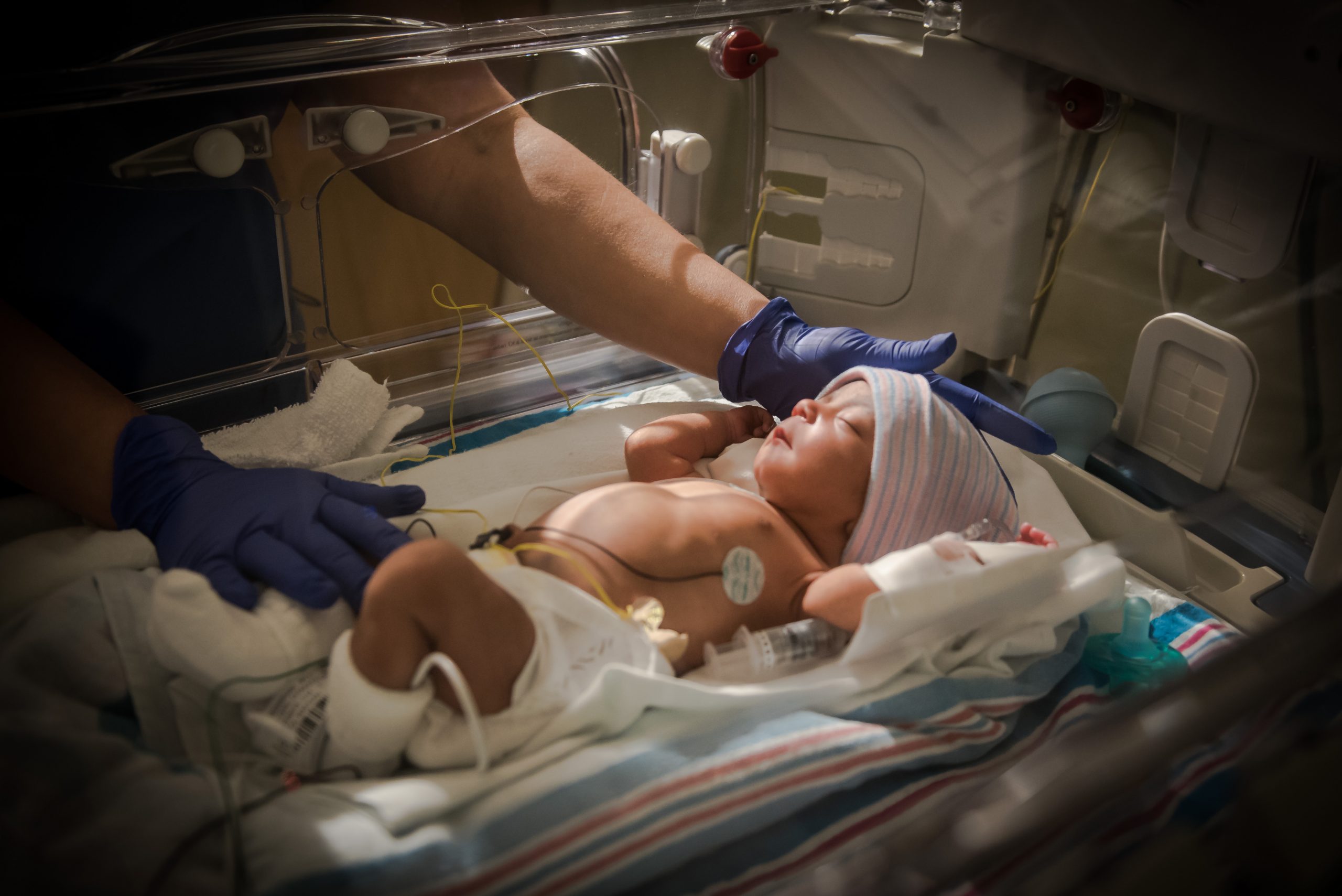 how to ensure the safety of families and babies during the COVID-19 pandemic.
how to ensure the safety of families and babies during the COVID-19 pandemic.
As a parent it can be hard to know that your baby may need specialized care or may have to spend time away from you. The Neonatal Intensive Care Unit, or NICU, is where premature babies and newborn babies who need special medical treatment are cared for. The NICU is comprised of a large and diverse team of specialized healthcare professionals that are dedicated to caring for the tiniest patients. Who is part of the NICU care team? There are many specifically trained specialists such as a Neonatologist (NICU doctors), Neonatal nurse practitioner, respiratory therapists, nurses, lactation consultants, speech/occupational/physical therapists, and more. It can be comforting to know that during this difficult time that there is a whole team giving their all to help care for your baby and offer you support.
In most cases, parents can be with their baby in the NICU at any time. The staff of the NICU will give you instructions on special hand-washing methods before entering the area. Parents are encouraged to take part in caring for their baby while staying there. The NICU team can help guide new parents on how to hold your baby if your baby needs extra care. Not only is this good for the parent’s mental health, but the contact will be able to soothe the baby and provide much needed bonding time. Now during a global pandemic, it is understandable that you may have concerns about keeping your baby safe from COVID-19. While COVID has altered our lives drastically it is still possible to bond with your baby in the NICU. Depending on the hospital you are staying with, the specific protocols may differ. If you are unsure about how you should bond with your baby, just ask the NICU staff! The healthcare team is there to make this experience as positive and beneficial as it can be for you and your baby.
NICU babies are our tiniest and most fragile patients. We have detailed protocols in place for handwashing and masking to ensure the health and safety of our NICU babies. Parents and family members can help protect our NICU babies against harmful viruses by receiving the COVID-19 vaccine. Breastfeeding mothers who have received the COVID-19 vaccine can pass along important virus fighting antibodies to their baby through breastmilk. You can reach out to your NICU team for guidance if you’ve been exposed to a virus or have flu-like symptoms.
Lastly, while you are caring for your baby don’t forget to check in with yourself. This is a stressful time, so it is okay to not be okay! Seek support from friends and family and other parents who have been through a NICU experience. If you need to speak to someone professionally about your mental health, your NICU team has resources for you. Remember you are not alone, there is a whole team of healthcare professionals waiting to help you navigate your time in the NICU.
Dr. Julie Gallois
 Dr. Julie Gallois is an Assistant Professor of Clinical Pediatrics in the Division of Neonatology at LSU Health Sciences Center and serves as a neonatologist at Touro and Children’s Hospital. A native of the greater New Orleans area, Dr. Gallois earned her medical degree and completed her pediatric residency, chief residency, and neonatology fellowship at LSUHSC School of Medicine. Dr. Gallois is board certified by the American Board of Pediatrics in General Pediatrics and board eligible in Neonatal-Perinatal Medicine. Her clinical interests include quality improvement, physician wellness and medical education. Her research interests include antibiotic effects of the neonatal microbiome. Dr. Gallois brings specific interest and skill in breastfeeding medicine, where she has been a leader in making hospitals more breastfeeding friendly for patient/families and employees and increasing breastfeeding education for staff and learners. She chose to work in the NICU because she wanted to make a difference for patients and families while treating them with skill, care, and understanding.
Dr. Julie Gallois is an Assistant Professor of Clinical Pediatrics in the Division of Neonatology at LSU Health Sciences Center and serves as a neonatologist at Touro and Children’s Hospital. A native of the greater New Orleans area, Dr. Gallois earned her medical degree and completed her pediatric residency, chief residency, and neonatology fellowship at LSUHSC School of Medicine. Dr. Gallois is board certified by the American Board of Pediatrics in General Pediatrics and board eligible in Neonatal-Perinatal Medicine. Her clinical interests include quality improvement, physician wellness and medical education. Her research interests include antibiotic effects of the neonatal microbiome. Dr. Gallois brings specific interest and skill in breastfeeding medicine, where she has been a leader in making hospitals more breastfeeding friendly for patient/families and employees and increasing breastfeeding education for staff and learners. She chose to work in the NICU because she wanted to make a difference for patients and families while treating them with skill, care, and understanding.
















